Have you heard of a pessary?
Do you have feelings of pressure and heaviness in the vagina at the end of the day or when working out? Do you leak urine with running or jumping activities? If you answered yes to either of those questions, then the first thing that you will want to do is get your pelvic floor assessed by a pelvic floor physical therapist.
To manage your symptoms your PT will want to assess and address how you are moving during exercise, how you are managing increases in intra-abdominal pressure, how you are breathing, and how your pelvic floor is responding to what you are doing. Along with addressing those factors, it may be helpful to add an additional layer of support to your pelvic floor depending on the severity of your symptoms. That’s where the pessary comes in!

What is a pessary?
A pessary is a small, silicone device that is inserted into the vaginal canal to help support the internal organs of the pelvis, including the bladder, vagina, uterus, and rectum. Pessaries are most often used to treat and help decrease symptoms of prolapse, but they can also help reduce urinary incontinence too.
This is a great non-invasive treatment for those who need extra pelvic support and for those that would like to avoid surgery! To find out if you may benefit from a pessary, you can use a temporary internal support, such as the “Poise Impressa” (see image below), to see if your symptoms of bulging, pressure, heaviness, or leaking are reduced. If they are, this could indicate that you would benefit from a pessary.

Who would benefit from a pessary?
If you have been diagnosed with a pelvic organ prolapse or experience stress urinary incontinence (leaking with coughing, sneezing, jumping, running) you may be a candidate for a pessary.
For incontinence, the pessary helps to elevate the bladder and puts the urethra (the tube through which we pee) into a better position.
For prolapse, the pessary supports the pelvic organs internally by placing support on the vaginal wall.
The type of pessary you need will depend on your symptoms and your diagnosis.
There are a select number of patients who may not be a good fit for a pessary including those who have a vaginal or pelvic infection and those who are unlikely to follow up with their provider after placement.
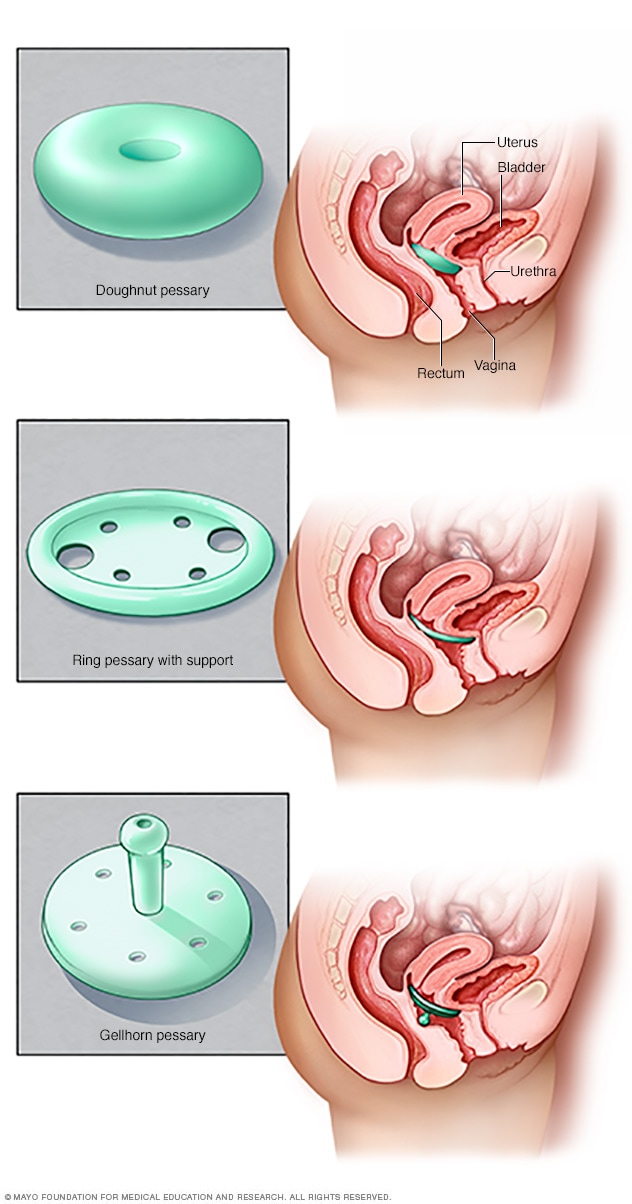
Where and how do I get a pessary?
Just like humans, pessaries come in all different shapes and sizes and the one that is best for you will depend on what needs to be “treated.”
Finding the right pessary for you may take some trial and error of several different kinds. There are a variety of sizes and styles that will need to be fitted and then worn to determine effectiveness. Effectiveness and the correct fit can be determined in your provider’s office immediately after placement by doing several tests and noting symptoms. Some of these tests may include sitting, standing, coughing, and bearing down. The device should not become dislodged during any of these movements. You should be able to void (pee) while wearing the pessary, if you are unable to do this then you may need a smaller size.
It is not uncommon to have to change the size of the pessary within the pessary fitting process (not just the day you get it) after the initial fit. Although the in-office tests will be done to assess the fit and size, it sometimes takes wearing it with more strenuous activity and with activities of daily living (picking up your children, household tasks, etc.) to most effectively determine the success of the pessary fit.
Managing your pessary.
It is imperative that throughout the process you are following up with your provider when they recommend it. Initially, it may be somewhat frequent to determine that your pessary is serving your needs and that your body is tolerating the device, and then less frequent as you become accustomed to it.
There are different types of options when it comes to pessaries, and it is best to speak to your provider about the pros and cons of each of them and what it will mean for your day-to-day life. Some are taken in and out daily (if you need extra support but just for exercise) and some can be left in for up to 3 months. If yours is the kind that can be left in (if it has drainage), then make sure to take it out at around the 3-month mark to clean it with soap and water. Some women choose to take it out, clean it, and then reinsert it themselves while others prefer to have the medical provider do it for them.
Pessaries can either be left in or taken out during intercourse, but most people find it more comfortable to remove them during sex.
Like with all interventions, there are many benefits but possibly some “downsides” of pessary use that need to be considered. The device may cause vaginal irritation, and some people may have increased vaginal discharge and odor. These complications should be managed with good vaginal and vulva hygiene and follow-ups with your provider. Long-term consequences are rare, however, neglect of the pessary could lead to infection or “impaction” in the vagina.

Closing thoughts
I highly recommended trying a pessary before surgery considering surgery if other conservative interventions have not worked for you. The benefits of a pessary over surgery include the following: it is non-invasive, there is no recovery time required, and they are less expensive. However, they are more upkeep and it can take some trial and error to find one that suits your needs.
This blog was written by our very own Pelvic/Women’s Specialist, Dr. Sam Greig.
References
- PennMedicine Women’s Health Blog 2016
- Viera et al. Practical Use of the Pessary. American Family Physician. 2000
* * *
Thanks for reading! If you’d like to learn more about who we are and what we do, click this link: https://upandrunningpt.com/