Pelvic floor
Have you heard about the pelvic floor and thought about its mysterious location “down there” but never really understood exactly what it is or what it does? As taboo surrounding discussing toileting and sexual habits decreases in the twenty first century, these terms are being thrown around a lot more than they used to and sometimes with little context or definition. So, ladies of Fort Collins, let’s learn more about it today!
The pelvic floor is a group of tendons, fascia, ligaments, and muscles that attach from the lowest part of the spine to the front of the hips and act and look like a hammock at the bottom of the pelvis or pelvic bowl. These muscles are under our conscious control which means that we can “ask” them to contract and relax – similar to how we can “ask” or control our elbow bending and straightening with the bicep muscle contracting and relaxing.
This group of muscles have an important role in support, stability, sexual function and maintaining urinary and bowel continence (“sphincteric”).
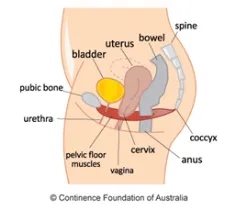
The pelvic diaphragm, or pelvic floor, helps to keep our pelvic organs supported and in place inside of our bodies. These organs can include the bladder, uterus and the bowel. When we have a lack of support for these structures from the pelvic floor, we may experience symptoms of vaginal or abdominal heaviness due to drooping of one of these organs onto the outside wall of the vaginal canal. These symptoms may indicate pelvic organ prolapse. Prolapse is fairly common, with increased occurance post vaginal delivery, however some women may be diagnosed with a prolapse and have no symptoms while others may have a very mild case with more severe symptoms.
The pelvic floor’s role in stabilityis that it is the bottom of the “core unit.” The core system is made up of four different muscle groups: 1. the diaphragm (our breathing muscle) on the top, 2. the pelvic floor on the bottom 3. the transverse abdominis (deepest layer of ab muscles) in the front and 4.the multifidi (spinal muscles) in the back. These muscles work together to help to maintain trunk stability while our arms and legs move, for example while running or while reaching for an object.
Although the pelvic floor muscles are not main movers for big movements, they need to work in synergy with other trunk muscles to create efficient movement patterns. So, when there is a dysfunction of the pelvic floor muscles, we may see dysfunction during movements which in turn may lead to restrictions in the ability to stay physically active¹.

During sexual activities and intercourse, contraction of the superficial pelvic floor muscles helps pump blood into the area which plumps the tissues and helps with arousal. Quick contractions of the pelvic floor muscles have been noted when one reaches climax. It is important to have the ability to contract these muscles as mentioned previously, however, it is equally important to be able to relax these muscles to minimize the chance of painful intercourse.

The muscles of the pelvic floor wrap around the urethra and the anus to help us maintain continent of pee, poop and gas throughout the day. We need to have enough strength in these muscles to overcome sudden increases in intra-abdominal pressure to maintain a dry state – such as not leaking with jumping or sneezing. However, we also cannot have these muscles so overused that they press on the bladder and cause overactivity of the detrusor muscle (bladder) which may cause us to run to the restroom 15x/day.
The pelvic floor is an awesome group of muscles with such a variety of functions that allow us to go about our day without noticing them – unless something goes wrong! And when things go wrong with the pelvic floor, unfortunately this can affect our quality of life. We can’t jump on the trampoline with our kids for fear of leaking or being intimate with our partner due to pain. So if you are experiencing any of these symptoms or you want to learn more about how to optimize your pelvic health and improve your quality of life – check us out at Up and Running Physical Therapy in Fort Collins, CO.
Reference:
- Evidence Based Physical Therapy Pelvic Floor Textbook, Kari Bo et al, pg 3

Dr. Sam Greig.
This blog was written by our very own Pelvic/Women’s Specialist, Dr. Sam Greig.